When you hear “robotic surgery,” does your mind conjure images of autonomous machines wielding scalpels, straight out of a sci-fi blockbuster? It’s a common, yet understandable, misconception. The truth, however, is far more grounded in human expertise and technological empowerment. Robotic surgery is not about replacing the surgeon; it’s about amplifying their skills to deliver unparalleled precision and improved patient outcomes.
But let’s be frank: how safe is it really? This question lingers in the minds of many considering advanced surgical options. To truly understand, we need to peel back the layers of innovation and explore the genuine interplay between human skill and robotic assistance.
Before we dive deeper, take a moment to watch our concise YouTube Shorts video that cuts through the initial myths and sets the stage for our detailed discussion. It’s a quick, insightful peek into what robotic surgery truly entails!
Table of Contents
What Exactly Is Robotic Surgery? Beyond the Buzzword
At its core, robotic-assisted surgery is a form of minimally invasive surgery where a highly trained surgeon utilizes a sophisticated robotic system to perform operations. The most widely recognized system, the da Vinci Surgical System, isn’t a robot that acts independently. Instead, it comprises three main components:
- The Surgeon’s Console: This is where the surgeon sits, viewing a high-definition 3D image of the surgical site and manipulating hand and foot controls to guide the robotic instruments. It’s akin to a highly advanced, immersive simulator.
- The Patient-Side Cart: Positioned next to the patient, this cart holds four interactive robotic arms that translate the surgeon’s movements into precise actions. These arms are fitted with specialized surgical instruments.
- The Vision System: A high-definition 3D camera provides a magnified, crystal-clear view of the surgical field, far superior to what the human eye can typically perceive during open surgery.
Imagine a surgeon with the steadiest hands, an eagle’s eye for detail, and instruments that can bend and rotate with greater dexterity than human wrists. That’s the essence of the robotic advantage.

The Unseen Hand: How Robotic Systems Elevate Surgical Expertise
The beauty of robotic assistance lies in its ability to augment, not replace, the surgeon’s capabilities. Here’s how:
- Enhanced 3D High-Definition Vision: Surgeons gain an immersive, magnified view of the operating field, providing unparalleled depth perception and clarity. This allows for meticulous identification of vital structures.
- Miniaturized, Wristed Instruments: The robotic instruments are incredibly small and feature seven degrees of freedom – far more articulation than the human wrist. This enables surgeons to maneuver in tight spaces with exceptional agility, performing intricate suturing and dissection.
- Tremor Filtration: Even the most experienced surgeons can have a natural, physiological tremor. Robotic systems filter out these micro-movements, ensuring rock-steady precision.
- Ergonomics for the Surgeon: Surgeons operate from a comfortable, seated position at the console, reducing physical fatigue during long and complex procedures. This sustained comfort can translate to more consistent performance.
These technological enhancements allow for operations to be performed through very small incisions, leading to a host of patient benefits.
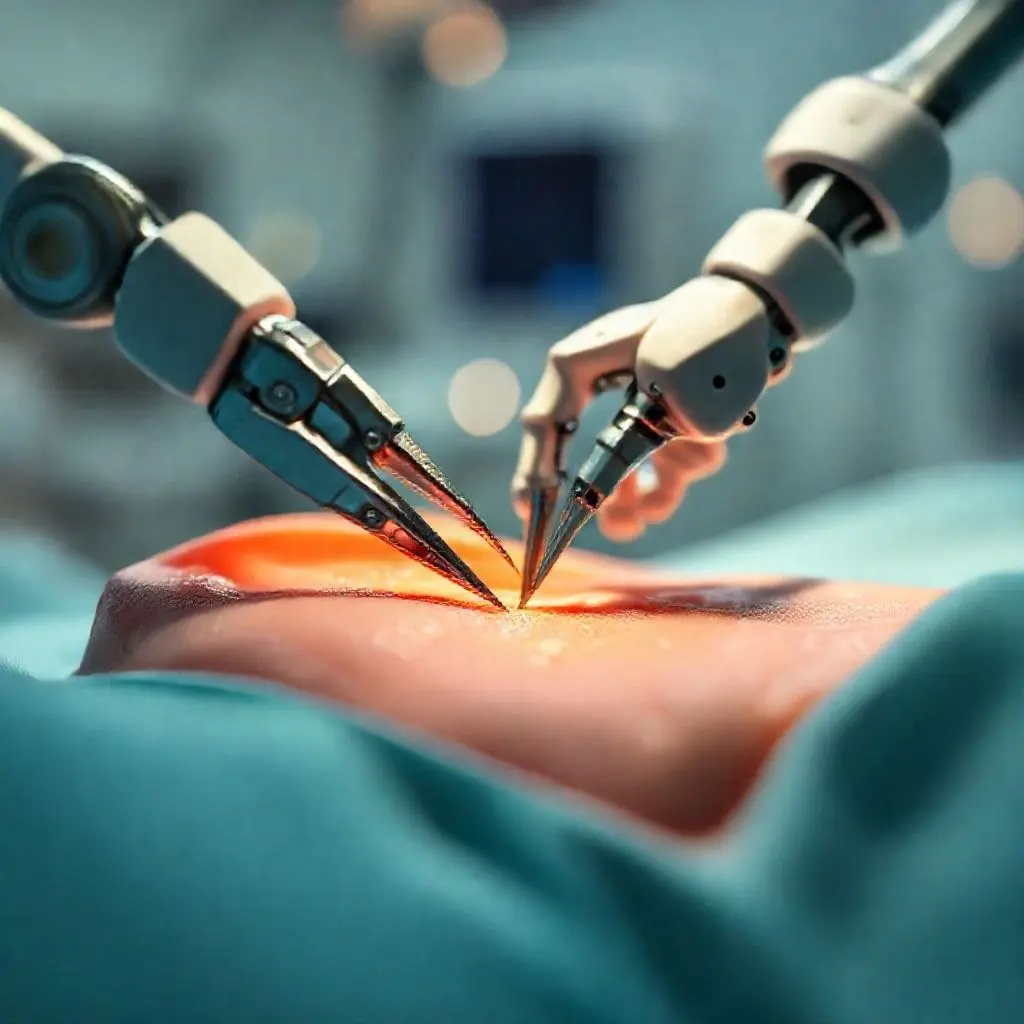
Patient Perks: A Smoother Road to Recovery
For patients, the advantages of robotic-assisted surgery often translate into a significantly more comfortable and quicker recovery experience:
- Smaller Incisions: This is perhaps the most visible benefit. Instead of a large cut, several small incisions (typically 8-12 mm) are made, leading to less tissue trauma.
- Reduced Blood Loss: The precision of the instruments and the clear visualization often result in significantly less blood loss during the procedure, lowering the need for blood transfusions.
- Less Post-Operative Pain: With smaller incisions and reduced internal tissue manipulation, patients typically experience less pain after surgery, often requiring fewer strong pain medications.
- Shorter Hospital Stays: Many patients can return home sooner, sometimes even the same day, compared to traditional open surgery.
- Quicker Return to Daily Activities: The faster recovery translates to patients getting back to their normal routines, work, and leisure activities much sooner.
- Lower Risk of Infection: Smaller incisions expose less internal tissue to the external environment, potentially reducing the risk of surgical site infections.
- Better Cosmetic Outcomes: For many, the smaller, less noticeable scars are a significant aesthetic benefit.

Safety First: Peeling Back the Layers of Risk and Reliability
This brings us back to the core question: how safe is robotic surgery? While no surgical procedure, regardless of technique, is entirely without risk, a growing body of scientific evidence consistently points to robotic-assisted procedures having safety profiles that are comparable to, and in many cases, superior to traditional open and even conventional laparoscopic methods.
Here’s why:
- Rigorous Training and Certification: Surgeons undergo extensive training and proctoring before they are certified to perform robotic procedures. This includes hours of simulation, supervised surgeries, and continuous education.
- Enhanced Visualization and Precision: As discussed, the 3D HD vision and articulated instruments allow for a level of precision that can reduce the risk of injury to surrounding tissues and structures. This is particularly crucial in complex anatomical areas.
- Controlled Environment: The robotic system operates within a highly controlled environment, with built-in safety mechanisms and continuous monitoring by the entire surgical team. The surgeon’s input is constantly required; if the surgeon removes their head from the console viewer, the system locks into place.
- Reduced Human Error (in some aspects): By filtering tremors and providing unparalleled visual detail, some elements of human error related to manual dexterity and visual acuity are mitigated.
Studies across various specialties – from urology (e.g., prostatectomy) and gynecology (e.g., hysterectomy) to general surgery (e.g., colorectal resections) – have demonstrated that robotic surgery can lead to:
- Lower rates of certain complications.
- Reduced need for blood transfusions.
- Shorter hospital stays.
- Improved functional outcomes for specific procedures (e.g., urinary continence and sexual function post-prostatectomy).
It’s important to remember that the safety of robotic surgery is inherently tied to the expertise of the surgical team and the specific procedure being performed. The technology is a sophisticated tool, and its effectiveness is maximized in the hands of a skilled and experienced operator.

Beyond the Hype: Dispelling Common Misconceptions
Let’s clarify a few persistent myths:
Myth 1: Robots operate autonomously.
Fact: Absolutely not. The robot is entirely dependent on the surgeon’s direct commands. Every movement of the robotic arms is a precise replication of the surgeon’s hand and foot movements at the console. It’s a master-slave system where the human is always the master.
Myth 2: It’s an experimental technology.
Fact: Robotic surgery has been around for over two decades. The first da Vinci system was cleared by the FDA in 2000, and since then, millions of procedures have been performed worldwide. It’s a well-established and continuously refined technology.
Myth 3: Robotic surgery is always more expensive with no real added benefit.
Fact: While the initial capital cost of the equipment is high, the overall cost-effectiveness can be favorable due to reduced hospital stays, fewer complications, and quicker patient recovery, which gets them back to productivity sooner. For many complex procedures, the clinical benefits justify the investment.
Where Robotic Surgery Shines: Key Applications
Robotic-assisted surgery has found its niche and often become the preferred approach for a wide array of complex procedures across various medical specialties:
- Urology: Prostatectomy (removal of the prostate), nephrectomy (kidney removal), partial nephrectomy (removal of part of the kidney), cystectomy (bladder removal).
- Gynecology: Hysterectomy (uterus removal), myomectomy (fibroid removal), ovarian cystectomy, pelvic prolapse repair.
- General Surgery: Colorectal surgery (bowel resections), hernia repair (inguinal, ventral), cholecystectomy (gallbladder removal), bariatric surgery.
- Cardiac Surgery: Mitral valve repair, coronary artery bypass grafting.
- Thoracic Surgery: Lung resections (lobectomy, segmentectomy) for cancer.
- Head and Neck Surgery: Transoral robotic surgery (TORS) for certain throat cancers.
The ability to operate with such precision in confined spaces makes robotic systems particularly advantageous for these delicate procedures.
Navigating the Nuances: Potential Risks and Limitations
Even with its impressive safety record, it’s crucial to acknowledge that robotic surgery, like any medical procedure, carries inherent risks and limitations:
- General Surgical Risks: These include risks associated with anesthesia, infection, bleeding, blood clots, and adverse reactions to medications. These are not unique to robotic surgery but apply to all forms of surgery.
- Longer Operative Times (initially): For surgeons in their learning curve, robotic procedures might take longer than traditional methods. However, with experience, operative times often become comparable or even shorter.
- Lack of Haptic Feedback: Unlike open surgery, where surgeons can directly feel tissues, most robotic systems do not provide tactile (haptic) feedback. Experienced robotic surgeons learn to compensate for this through visual cues and instrument tension.
- Cost to the Healthcare System: The initial investment in robotic systems and ongoing maintenance costs can be substantial for hospitals, though as mentioned, this can be offset by long-term patient benefits.
- Not Universally Applicable: Robotic surgery isn’t suitable for every patient or every type of procedure. The surgeon will determine if it’s the best approach based on individual patient factors and the specific condition.
Open and honest discussion with your surgeon about these factors is paramount.
Choosing Wisely: What to Consider for Robotic-Assisted Procedures
If robotic surgery is an option for your condition, consider the following:
- Surgeon’s Experience: Inquire about your surgeon’s specific experience with robotic surgery, including the number of procedures performed and their success rates for your particular condition. Look for board-certified surgeons with specialized training.
- Hospital Volume and Expertise: Hospitals that perform a high volume of robotic surgeries generally have more experienced staff and robust support systems in place.
- Discussion of Alternatives: Your surgeon should thoroughly discuss all available surgical options, including open and conventional laparoscopic techniques, along with their respective risks and benefits.
- Understanding Your Specific Condition: Ensure you have a clear understanding of why robotic surgery is being recommended for your unique situation and what outcomes you can realistically expect.

Looking Ahead: The Human-Machine Symphony
The journey of robotic surgery is a testament to how human ingenuity continues to push the boundaries of what’s possible in medicine. It’s a powerful partnership between a highly skilled surgeon and advanced technology, working in concert to achieve outcomes that were once unimaginable.
So, the next time you wonder about the safety of robotic surgery, remember this: it’s not robots replacing surgeons; it’s cutting-edge technology empowering them. It’s about precision, reduced invasiveness, and a commitment to helping patients heal faster and with greater comfort. The future of surgery is not just about innovation, but about intelligent integration that puts patient well-being at the forefront, ensuring you are truly in the steadiest hands – both human and mechanical.
Frequently Asked Questions About Robotic Surgery Safety
1. Is robotic surgery more expensive for the patient?
Generally, for the patient, the out-of-pocket cost for robotic surgery might be comparable to other surgical methods, depending on your insurance coverage, deductibles, and co-pays. While the equipment itself is expensive for hospitals, these costs are often absorbed into standard procedure fees. Furthermore, shorter hospital stays and quicker recovery can indirectly reduce overall patient costs by minimizing lost wages and post-operative care needs. It’s best to discuss specific cost implications with your insurance provider and the hospital’s billing department.
2. How long does recovery take compared to open surgery?
Recovery time for robotic surgery is typically significantly shorter than for traditional open surgery. Due to smaller incisions and less tissue trauma, patients often experience less pain, require fewer days in the hospital, and can return to normal daily activities within weeks rather than months. For example, a robotic hysterectomy might allow a patient to return to light activities in 2-3 weeks, compared to 6-8 weeks for an open procedure. Individual recovery times can vary based on the type of surgery, patient health, and adherence to post-operative instructions.
3. Can any surgeon perform robotic surgery?
No. While many surgeons are embracing robotic technology, it requires specialized, rigorous training and certification. Surgeons must complete extensive training programs, including simulation exercises and supervised procedures, to become proficient and credentialed in robotic surgery. It’s crucial to choose a surgeon with significant experience and a proven track record in the specific robotic procedure you are considering.
4. What happens if the robot malfunctions during surgery?
Robotic surgical systems are designed with multiple layers of safety redundancies and protocols. If a malfunction or power interruption occurs, the system is designed to safely pause or cease operation, allowing the surgical team to intervene. The surgeon is always present at the operating table and can quickly transition to a conventional laparoscopic or even open surgical approach if necessary. Such malfunctions are rare, and the primary concern remains patient safety, with the human surgical team always having ultimate control and backup plans.
5. Are there any conditions where robotic surgery is *not* recommended?
Yes, robotic surgery is not suitable for all patients or all conditions. Factors that might make it less ideal include very complex or extensive cancers, previous extensive abdominal surgeries leading to significant scar tissue (though this can often still be managed), certain types of emergencies, or patients who cannot tolerate the specific positioning or insufflation (gas inflation) required for robotic procedures. The decision for robotic surgery is always made on a case-by-case basis by the surgical team, considering the patient’s overall health, the specific pathology, and the surgeon’s expertise.